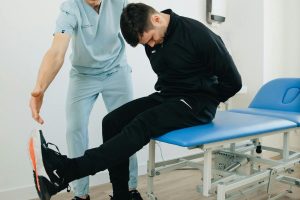
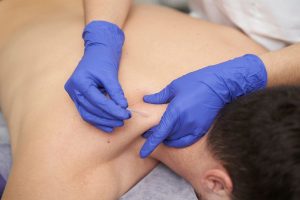
Throughout our lives, it’s common at some point to have a workplace injury that requires the use of workers’ comp insurance, a safety net designed to provide financial support during recovery. As physical therapists, we often field questions from those patients in our clinics (as well as develop and facilitate their recovery plans).
For those undergoing physical therapy, one of the most common questions is: How long will workers’ comp pay for physical therapy?
While there’s no short answer, we can provide some guidance on this subject:
Workers’ comp generally covers physical therapy as long as it is deemed medically necessary for the injured employee’s recovery. The duration for which workers’ comp pays for physical therapy varies and depends on factors such as the severity of the injury, the prescribed treatment plan, and the individual’s progress in rehabilitation.
Below, we’ll delve into the factors that influence the duration of physical therapy coverage under workers’ compensation and offer insights to help individuals navigate the process effectively.
Understanding Workers’ Comp and Physical Therapy
Workers’ compensation is a state-mandated insurance program that provides medical and wage benefits to employees who sustain work-related injuries. Physical therapy, a crucial component of rehabilitation, is often recommended to restore function and mobility.
For more information on whether or not physical therapy is right for you, see our full article on whether or not you need physical therapy after a work injury.
The duration of physical therapy coverage under workers’ comp varies, and several factors come into play:
1. Severity of Injury
The extent of your injury significantly impacts the duration of workers’ comp coverage for physical therapy. Severe injuries may require more extended rehabilitation, leading to an extended coverage period.
2. Prescribed Treatment Plan
Your treating physician will develop a customized treatment plan based on the nature of your injury. The type of treatment prescribed will depend on the nature of your injury. The duration of physical therapy coverage is often aligned with the recommended treatment timeline outlined in this plan.
3. Medical Necessity
Workers’ comp pays for treatments deemed medically necessary. If your healthcare provider determines that continued physical therapy is one of the medical treatments for your recovery, the coverage is likely to be extended.
4. Progress and Improvement
Workers’ comp coverage for physical therapy is typically contingent on the demonstrable progress in your recovery. If you are making significant strides and meeting rehabilitation goals, the coverage may continue. Conversely, if little progress is observed, adjustments to the treatment plan may be necessary.
5. Duration Limits
Some states impose specific time or visit limits on workers’ comp coverage for physical therapy. Familiarize yourself with the regulations in your state to understand any potential restrictions.
Does Physical Therapy Increase Workers’ Comp Settlements?
While physical therapy is often a crucial component of rehabilitation, leading to improved functionality and recovery for injured workers, its direct correlation to settlements is not guaranteed.
The impact of physical therapy on workers’ compensation settlements can vary, but it is possible for adherence to a physical therapy regimen to increase workers’ compensation settlements in some cases.
The reason for this is that effective physical therapy can positively contribute to a case by demonstrating a commitment to rehabilitation, potential improvement in functionality, and reduced long-term disability, which may, in turn, influence settlement negotiations.
Settlement amounts in workers’ comp cases are typically determined by factors like the extent of permanent disability, medical expenses, and the impact of the injury on the individual’s ability return to work.
However, each case is unique, and the influence of physical therapy on workers’ comp settlements is best assessed in conjunction with legal advice and a thorough understanding of the specific circumstances surrounding the injury.
If you’re interested in increasing your settlement, a good workers’ compensation attorney is likely your best asset.
Does workers’ comp pay for time off for physical therapy?
Whether workers’ compensation covers time off for physical therapy, most of the time, depends on a demonstrated medical necessity for the treatment. If a healthcare provider deems time off for physical therapy as essential for the injured worker’s recovery, and it aligns with the prescribed treatment, there is a higher likelihood of workers’ comp covering the associated time off.
Additionally, Temporary Total Disability (TDD) benefits may provide compensation for lost wages during the period where the employee is unable to work due to the injury. This can include time off for physical therapy.
Employers’ policies and state regulations further contribute to determining the extent of coverage for time off related to physical therapy under workers’ compensation.
Whether the workers’ compensation benefits continue to pay largely depends on the adherence to the prescribed treatment plan, and the quality and timeliness of the reporting.
Three tips for maximizing workers’ comp coverage
1. Open communication
Maintain open communication with your healthcare provider and workers’ comp case manager. Regular updates on your progress and any challenges you may be facing can contribute to a smoother process.
2. Adhere to your treatment plan!
Adhering to your prescribed treatment plan is crucial. Attend all scheduled physical therapy sessions and follow the recommendations provided by your healthcare team.
3. Timely reporting
Report any changes in your condition promptly to both your healthcare provider and workers’ comp representative. Timely communication ensures that adjustments can be made to your treatment plan if necessary.
Maximizing worker’s compensation for physical therapy
While the coverage of time off for physical therapy under workers’ compensation can be influenced by various factors, understanding the key elements and actively participating in the process can help ensure you receive the support you need during your recovery.
By staying informed, communicating effectively, and adhering to prescribed treatment plans, you can navigate the complexities of workers’ comp and prioritize both your health and professional well-being.