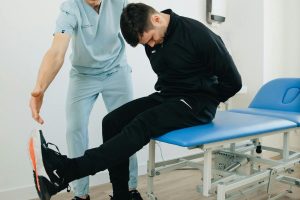
Jeff Petersen took some time this week to discuss how to reduce fall risk in older individuals. In the video, he discusses risk factors such as balance issues, previous falls, and medical conditions like arthritis or vision deficits. He also discusses the systems involved in balance and provides some self-assessment tools for balance and fall risk. If you prefer to read instead of watch, scroll down for a transcript.
Additionally, see our written guide to home fall risk assessment, and our guide detailing how fall risk factors are classified by professionals.
Here’s the video:
The following is a transcript of the video below discussing how to reduce fall risk in older individuals.
Hello, my name is Jeff Petersen, owner of Petersen Physical Therapy. We’re going to talk today about falling, and risk of falling, and how to decrease your risk of falling. I want to talk about falling because one in three older adults will suffer a ground level fall. What happens is it creates a cycle of falling, where a person will fall, and maybe get hurt. Not a life threatening injury, but an injury enough that then they have decreased activity because they are afraid to fall. Decreased activity leads to decreased muscle strength and joint flexibility, which actually increases your risk of falling.
So, one of the best things to do to combat the risk of falling is to get up and move around. We want to make sure that you do it safely. I want to first talk about why people fall. Balance is a complex mechanism. It’s about receiving the information from the environment, integrating that information, planning the movement, and executing the movement. All of that happens instantaneously, without conscious thought.
There are many systems that are involved:
- Your musculoskeletal system is involved – that’s your joints and your tendons and your muscles.
- Your vestibular system is involved – which is your inner ear, and the integration of what you see.
- Your visual system is involved.
- Your neurological system is involved – your central neurological system – your brain, your processing, and the nerves that go out to the joints and the muscles and the tendons.
So, it’s a really complex mechanism, and it’s amazing that we can get up and walk and not fall because it is so complex; you see it with children.
What happens is as we get older, there are some risk factors. If we’re on medication, that can cause a decrease in balance and lead to a higher risk of falling:
Important fall risk factors
- If you have weakness in your lower extremities.
- A previous fall is always a risk factor.
- A vision deficit.
- Arthritis.
- If you’ve noticed you’ve decreased your activities of daily living and not getting up as much.
- Cognitive deficit.
- One of the biggest things, too, is age. As we get older, even starting to hit 60.
One of the stories that I was telling a patient was that I walk my dog. I walk my dog at dusk, and all of a sudden I noticed that I tripped over the speed bump that we have in our neighborhood because visually, I couldn’t quite differentiate that. Now, when I was a 25 year old man, that never would have happened. Now that I’m pushing 60, I have to be a little bit more careful and watch where I step.
The biggest concern that I have for people that may have some of these risk factors is they get embarrassed and they don’t want to talk about it, and they don’t want to think about it. There’s no reason to be embarrassed if you’ve had a ground level fall. There’s no reason to be embarrassed if you’ve noticed that your balance is starting to decrease a little bit. It’s really important to take care of.
Again, one of the best ways to take care of it is through activity and exercise. So, if you’re unsure of what to do, you can always see your physical therapist or your physician. We have plenty of exercises that we can share with you. There’s also some things you can do to check your own balance.
Fall risk assessment at home
One thing is to see if you’re having difficulty standing from a seated position. If you notice it’s more difficult to get up when you’re sitting. The other one is if you have difficulty or hesitance to walk up and down stairs. Another one is just a single leg balance test. So, you stand on one leg in the corner of two counters and you see how long you can stand on one leg without having to put the other foot down. If you can’t stand on one leg for at least 10 seconds, that’s an indication that you might be at risk of falling.
It’s important to do those self assessments, and it’s really important to open a dialogue with your physician and your physical therapist. If you have questions or concerns you can always see us.
In the next article, we are going to assess a piece of equipment that we have here. It’s called the 60 Up. I was watching TV late one night and I couldn’t sleep. I got up and put the TV on and I see a commercial with Bob Eubanks with the 60 Up. I was intrigued by the piece of equipment, and I thought, let’s take a look and see if this is something that might be helpful for people to work on their balance, and on their lower extremity strengthening at home. So look out for our next post, which will be a review of the 60 Up exercise equipment.
As always, if you need assistance or would like an evaluations, contact us or call us today!