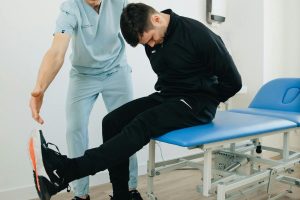
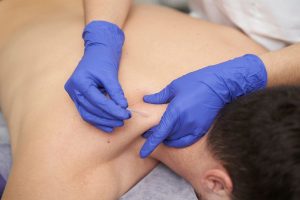
Though our practice has contracts with almost every major insurance company, there are still sometimes situations where out-of-network physical therapy billing makes the most sense.
Out-of-network physical therapy makes the most sense when you require specialized care not available within your insurance network, have a strong preference for a specific therapist, or prioritize personalized treatment.
In this article, we’ll discuss the situations in which you may find it beneficial to bill insurance out-of-network for physical therapy, and discuss the pros and cons of doing so.
What does out-of-network physical therapy mean?
The term out-of-network physical therapy refers to receiving rehabilitation services from a licensed physical therapist who is not part of your health insurance plan’s network.
Typically, health insurance plans will have a network of preferred healthcare providers with whom they have negotiated payment rates. This is, of course, a win for you. However, sometimes we’ve got a specific treatment modality in mind that a given in-network therapist doesn’t have training in, or we’ve received a specific referral from a friend or physician to a certain physical therapist that is not part of the preferred network.
This is most useful in cases where you’re looking for a highly specialized treatment, such as pelvic floor therapy, hand therapy, or Ehlers-Danlos therapy.
Many insurance companies have an “out of network” rate that they’ll pay, although the out-of-pocket costs for physical therapy may be higher.
You can typically discover your insurance plan’s out-of-network payment rate by simply calling them to ask. Alternatively, you could have the physical therapist you’re planning to see verify your insurance coverage and provide you with a detailed statement as to what kind of coverage you can expect if you seek treatment with them.
The drawbacks of typical in-network physical therapy
The obvious downside of the “in-network” system is that you’ll have a more limited pool of options to choose from. If the physical therapists in your area don’t specialize in the form of treatment that you’re looking for, or if the one you wish to use isn’t in-network, then you’re stuck.
Additionally, therapists can sometimes be hamstrung by the fact that they’ll have to bias their treatment towards using modalities they know insurance companies will pay for. This can vary from insurance company to insurance company and can become very cumbersome.
Therapists want to see you recover, but they also want to be compensated for their time. When doing a lot of work through insurance, it can be much harder for therapists to make ends meet, and they need to make up for it in extra volume.
Don’t get us wrong, our physical therapists do their best and they are top-notch providers. However, there’s simply less wiggle room for individualized attention once insurance gets involved.
Out-of-network physical therapy as a potential solution
Since Arizona is a direct-access state, physical therapists here can see anyone who comes to them, even without a referral. This means that if you’ve decided you want to see one of our therapists for any reason in particular, you can simply call our office and schedule an appointment.
Though this “direct access” channel is independent of the decision to use on in-network provider, you are also free to bill out-of-network or simply choose a cash-pay option in order to allow you and your therapist to have full control over the treatment you’ll receive, how long it will last, and the amount of attention you need.
Benefits of physical therapy out of network
Out-of-network physical therapy can have a number of benefits, depending on what you’re looking for.
If you’re paying out of pocket for an out-of-network physical therapy practice, it can provide greater freedom to the therapist to give you hands-on attention. Also, the lack of required insurance authorization can lead to reduced wait times to get started and greater flexibility in scheduling.
Sometimes, a therapist will also have more ability to explore alternative treatment options with you, rather than having to stick with whatever modalities your insurance company will pay for.
Also, many insurance companies have a cap on the number of visits or the total amount they’ll pay in a certain year. If you decide to seek physical therapy out of network, then you’ll get to seek as much treatment as you need, without having to worry about being discharged prematurely simply because your insurance benefits ran out.
Potential drawbacks of going out of network
The drawback of going out of network for physical therapy (or any healthcare service) is that your out-of-pocket costs for physical therapy are going to be higher by default.
You’ll be relegated to either cash-only physical therapy practices or out-of-network insurance billing.
Insurance companies typically aren’t willing to pay as much for out-of-network providers, and reimbursement can take longer.
It’s also worth mentioning that the onus will be on you to discuss and sign the particulars of your payment arrangement with your physical therapist on the front end to avoid any unpredictable expenses during the process.
Should you choose out-of-network physical therapy?
The decision to opt for out-of-network physical therapy services ultimately depends on your unique healthcare needs, preferences, and financial situation.
While out-of-network care can offer benefits such as specialized expertise, personalized treatment, and quicker access to certain therapies, it comes with the notable drawback of higher out-of-pocket costs.
Before making this choice, make sure that you know what your out-of-network benefits are by either calling your insurance company or having your physical therapist verify your coverage. From there, you can decide to cash pay for physical therapy, bill out-of-network, or seek another health care provider.